The optimal duration of thromboprophylaxis has also been assessed in patients undergoing HFS. In a cohort study of 897 HFS patients who received perioperative prophylaxis with enoxaparin, 40 to 60 mg per day for about 5 weeks, objectively confirmed, symptomatic VTE occurred in only 7 patients (0.8%), with no cases of PE. However, major bleeding was encountered in 5% of patients, including 5 cases of intracranial bleeding (2 patients had intracranial hemorrhage that may have directly related to the drug and 3 patients had ICH subsequent to the fall and 20 cases (2.2%) of wound hematomas requiring surgical evacuation. A recent double-blinded clinical trial provided 656 HFS patients with fondapa-rinux, 2.5 mg SC once daily for about 7 days, followed by randomization to continuation of prophylaxis with fondaparinux or placebo for an additional 3 weeks. Venography, performed after 4 weeks of prophylaxis, documented DVT in 1.4% of the extended prophylaxis patients and in 35.0% of placebo recipients (RRR, 96%; p < 0.001). The rates of symptomatic VTE were 0.3% and 2.7%, respectively (RRR, 89%; p = 0.02). Bleeding rates were not significantly different.
Canadian Health and Care Mall
The results of a number of economic studies have suggested that extended, post-hospital discharge prophylaxis may be cost-effective in comparison with in-hospital prophylaxis. Based on all of the data about duration of prophylaxis in orthopedic surgery, patients undergoing major orthopedic surgery should receive prophylaxis with LMWH, fondaparinux, or a VKA for at least 10 days. Given that current hospital stays are generally < 5 days, this recommendation implies that post-hospital discharge prophylaxis should be provided to most pa-tients. For patients undergoing THR or HFS, more prolonged prophylaxis for up to 28 to 35 days is recommended for those patients who are considered to be at high risk for VTE. Although further studies are needed to define who is at high risk, factors shown to predispose patients to VTE following major orthopedic surgery include a history of VTE or current obesity, delayed mobilization, advanced age, or cancer. Other risk factors that might be clinically important include a history of congestive heart failure or COPD, as well as female gender. The extended use of a VKA (INR target 2.5, range, 2.0 to 3.0) is an acceptable alternative to LMWH, although the incidence of major bleeding may be higher with oral anticoagulants. The pentasaccharide fondaparinux is recommended for extended prophylaxis following HFS. The use of either LMWH or an oral VKA also may be effective in HFS patients, although prolonged use of these agents has not been properly studied in this patient group.
Recommendations: Duration of Prophylaxis
1 We recommend that patients undergoing THR, TKA, or HFS receive thromboprophylaxis with LMWH (using a high-risk dose), fondaparinux (2.5 mg daily), or a VKA (target INR, 2.5; INR range, 2.0 to 3.0) for at least 10 days (Grade 1A).
2 We recommend that patients undergoing THR or HFS be given extended prophylaxis for up to 28 to 35 days after surgery (Grade 1A). The recommended options for THR include LMWH (Grade 1A), a VKA (Grade 1A), or fondaparinux (Grade 1C + ). The recommended options following HFS are fondaparinux (Grade 1A), LMWH (Grade 1C+), or a VKA (Grade 1C+).
3 Elective spine surgery
Unfortunately, most data about thromboprophylaxis in patients undergoing elective spine surgery come from small, retrospective studies of poor methodological quality. Although the incidence of VTE in these patients appears to be considerably lower than that following major lower extremity surgery, some patients seem to be at high enough risk to consider prophylaxis. A systematic review of 20 studies reporting complications after lumbar spinal fusions noted a 3.7% incidence of symptomatic DVT and a 2.2% rate of PE. In the only two studies that performed routine venography in patients undergoing spine surgery who did not receive VTE prophylaxis, DVT was detected in 18% of the 205 patients. In one of these studies, increased age and surgery of the lumbar spine (21%) vs surgery of the cervical spine (6%; p = 0.003) were independent predictors for DVT. Other possible risk factors include an anterior or combined anterior/posterior surgical approach (possibly related to intraoperative manipulation of the iliac veins or inferior vena cava), surgery for malignancy, a prolonged procedure, and reduced preoperative or postoperative mobility.
Symptomatic VTE and fatal PE are occasionally observed in spinal surgery patients despite prophylaxis using IPC and/or GCS.
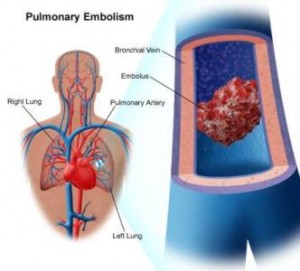
Symptomatic VTE and fatal PE
In a prospective but observational study of 306 patients undergoing elective spinal surgery, venographic DVT was found less frequently in patients who received IPC (6%) than in those who had received no prophylaxis (21%). DUS identified DVT in 2% of 1,527 spinal surgery patients from 11 prospective studies, all of whom routinely used mechanical prophylaxis. Unfortunately, the absence of control subjects in these studies prevents one from validly estimating the degree of protection afforded by mechanical prophylaxis in this patient group. In one small clinical trial, no cases of symptomatic VTE or abnormal DUS findings were noted among any of the 110 patients randomized to receive prophylaxis with GCS alone, GCS plus IPC, or GCS plus warfarin. Another randomized clinical trial compared LDUH with no prophylaxis among 38 laminectomy patients, using the FUT to screen for thrombosis. DVTs were detected in none of the 18 LDUH patients and in 5 of 20 control subjects. Another small clinical trial randomized spinal surgery patients to receive enoxaparin, 40 mg SC daily, or IPC. No venographically detected DVTs were detected in any of the 30 patients who received enoxaparin, and in 3 of the 30 who had received prophylaxis with IPC.